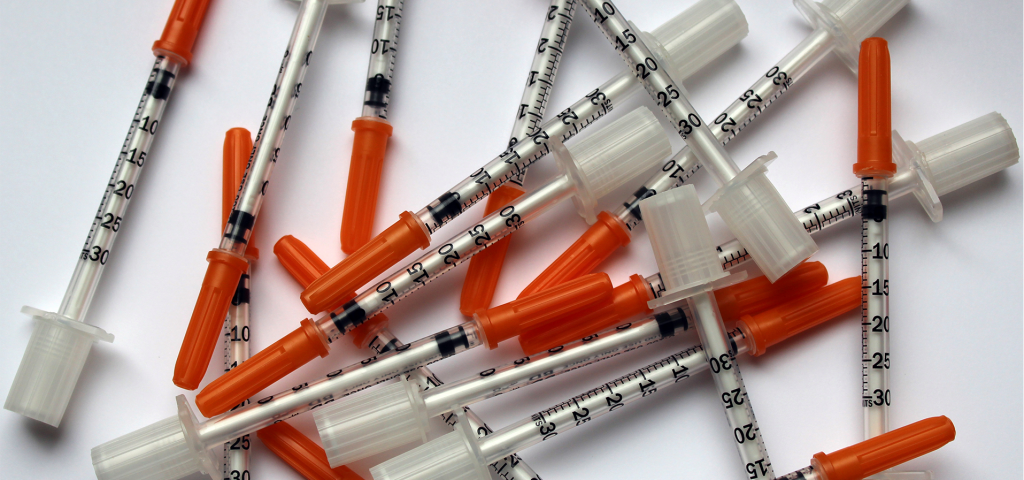
Drug overdose deaths in 2017 reached a record 72,000 according to preliminary data from the Centers for Disease Control and Prevention, two thirds of these deaths were linked to opioids. With the death toll rising, policymakers are desperate for anything that may help. Those who advocate for addiction and mental health reform are continuing to challenge the criminalized framing, arguing that if the goal is to save lives from addiction and overdose, a more compassionate approach is necessary. But what is the difference between compassionate and enabling? That’s the big debate when it comes to safe injection facilities. To many it sounds counterproductive, a place for people addicted to drugs to go and safely shoot up with clean needles and nurse supervision, but safe injection sites help decrease the number of overdoses and the spread of diseases such as Hepatitis and AIDS in the intravenous drug users communities for the past 30 years.
There are over 100 safe use sites operating in nine countries around the world, Switzerland opened the first one in 1986 and Germany, the Netherlands, Norway, Luxembourg, Spain, Denmark, Australia and Canada followed suit. The first North American supervised injection site, opened in Vancouver, Canada in 2003. Within two years overdose deaths dropped by 3% according to The Drug Policy Alliance. Vancouver’s InSite program, exempt from federal drug laws, is located in a downtown building where drug users have access to 12 private booths to inject drugs such as heroin or cocaine. In 2016 over 5,000 users were referred to other social/health services. InSite also intervened in over 1,000 overdoses, which could have been fatalities without the site’s services. Safe sites are a form of harm reduction, which means it is put in place to lessen the negative consequence of a behavior. Harm reduction in substance abuse can often get a bad reputation, people on Subutex for years, or people taking the “easy way out” of getting clean and sober. Harm reduction isn’t meant to be an easy way out, it is put in place to help people stay safe. The nurses and social workers who work here are ready to send anyone who is looking for help, to treatment. You cannot choose to go to treatment if you die from an overdose.
The United States has been playing with the idea of safe sites for the past couple of years, in fact Seattle, Washington officials approved the nation’s first site back in January 2017 in a unanimous vote of the King County Board of Health. Massachusetts, New York, Maryland, New Hampshire and Vermont are among the other U.S cities exploring this option. However, none of these cities would be the first in the US to open a safe injection site. There have been numerous underground facilities operating in the country for years. In Brooklyn, NY, there is a “secret site” where people go for a clean needle exchange. They then use the bathroom, were they are monitored by audio and able to use their drug of choice. The facility operator then listens to make sure you are safe in the bathroom. After you then dispose of your needle properly. The facility operators, who study harm reduction, have Narcan on hand in case of an overdose and information on treatment available.
Safe sites status as illegal under the Controlled Substance Act isn’t worrying the people pushing these sites, as they believe the good outweighs the bad when it comes to aiding in overdose prevention, the spreading of infectious diseases like AIDS and Hepatitis, and helping people get into treatment centers.
Seattle Ex-Mayor Ed Murray believed this was a necessary step in reducing deaths in the state of Washington. “These sites save lives and that is our goal in King County,” Murray said in a statement. Although there is no funding for these sites yet, two were approved in both Seattle and King County. King County Board of Health voted on the safe use sites and King County Executive Dow Constantine and Mayor Ed Murray gave them final approval. Funding for these sites is still unknown, however in a statement made this June by the Seattle Human Services Department, “safe-use vans” will be rolling out within the next year. It will cost an estimated 1.8 million dollars to fund the safe-use vans, which will be considered a King County Public Health ran facility. The van will park in one spot, daily, and will be a place for people to safely inject drugs. There will be social workers, nurses and other professionals working in the van to help support the substance users by connecting them to treatment and making sure they are safe from HIV and other infections, as well as helping aid in overdose prevention.
However, in the northeast progress has been slower. Vermont was one of the states looking into safe injection facilities, until the Attorney General shot down their research and interest. In a statement last year about a proposal to open supervised consumption sites in Vermont, the Justice Department warned that the facilities “would violate federal law.” The Justice Department claimed in a statement, “It is a crime, not only to use illicit narcotics, but to manage and maintain sites on which such drugs are used and distributed.” In the neighboring state of New Hampshire, Tim Lahey, a physician at Dartmouth-Hitchcock Medical Center, and the director of education at the Dartmouth Institute for Health Policy and Clinical Practice, believes that safe injection sites should be open in hospitals. He thinks it would help the addict to be in a hospital setting and would be viewed as more acceptable since it would be a hospital setting.
In big cities, like Boston and New York, they are less concerned about the federal law and more concerned with saving the lives of the people using these dangerous drugs.
Massachusetts Senator William Brownsberger proposed a bill for safe sites in Boston that has passed, known as S.2508, which gives the state of Massachusetts authorization to investigate if safe sites would work. The Senator strongly believes that, “Safe injection facilities are one possible tool we have to try to stop the deaths from fentanyl. Whether we can get one running in Massachusetts and whether it would work as we might hope remains to be seen.” While many people in Boston are against these sites, Dr. Jessica Gaeta, chief medical officer at the Boston Health Care for the Homeless, has been promoting a similar way to aid in the fight against the opiate epidemic. In March 2016, Gaeta initiated a program that she calls a “safe place.” This facility has chairs where addicts can sit while a nurse monitors vital signs. They can also administer Naloxone in case of an overdose. Gaeta said 400 people had used the facility and about 10% of them have gone directly from the room into treatment. Healthcare for the Homeless has an annual budget of approximately $50 million, about 75% of that comes from third party reimbursements from MassHealth, Medicare and Health Safety Net. The difference between Gaeta’s room is that patients are not be permitted to get high on site, making it less taboo and more in line with federal laws. Massachusetts is in dire need of a new approach considering the 1,990 confirmed opiate related deaths in 2016, according to the Department of Public Health.
In the neighboring state of New York, The New York Daily News reported that the City Council approved $100,000 to study whether to set up safe sites. The $100,000 comes from a $5.6 million budget the city currently has in place to fight against AIDS. According to New York Daily News, the funding was approved by the City Council in September 2016, but nothing has been built yet. Mayor Bill De Blasio said in a statement that, “After a rigorous review of similar efforts across the world, and after careful consideration of public health and safety expert views, we believe overdose prevention centers will save lives and get more New Yorkers into the treatment they need to beat this deadly addiction.” The study will be run by the Health Department and will look at the feasibility of NYC having a safe use site.
In Maryland, one man is pushing for harm reduction and safe injection sites. State House of Delegates member, Dan Morhaim, is also an emergency physician who has seen the opiate epidemic continue to grow. He says he has administered Narcan “many times,” which is why he is pushing for safe injection sites. Morhaim believes his bill for supervised injection sites is just one of many creative approaches that will be needed to solve the heroin problem throughout Maryland. “It’s not going to cure everyone,” he said. “But moving people from more dangerous behavior to less dangerous behavior is progress.”
In cities like Philadelphia, where the epidemic screams to be seen, as homeless set up camps in Kensington square, needles flood the street, they are committing to change, they are committing to saving lives. Given the scope and devastation of the opioid crisis, which has claimed approximately 1,200 lives in 2017, Philly created a comprehensive, 18-point plan to address the different ways this epidemic is affecting our residents and how to help.
Comprehensive User Engagement Sites, known as CUES, are safe injection facilities the city is planning to open up. The CUES are not the only answer, but one option that can help people struggling with substance use disorder stay alive long enough to get into treatment. We know that its possible for people fighting addiction to recover, and it is in everyone’s best interest to make sure that our residents stay alive long enough to get there.
Research suggests that safe sites can be an effective public health strategy. Providing clean needles helps prevent infectious diseases like HIV and Hepatitis C from spreading. When combined with a suite of supportive services for homeless or addicted people looking for help, safe injection sites can create a life-saving pipeline between an addicted population and community health professionals.
Safe-use sites are an important key to the harm reduction method. It is something that needs to be considered in the U.S when dealing with addiction if we want to see the rising number of overdoses go down during this public health crisis. It is also a great way to get those who are still using drugs, to think about or even know about the different treatment options that are available.